Tibialis Posterior Tendon Dysfunction (Acquired Flatfoot)
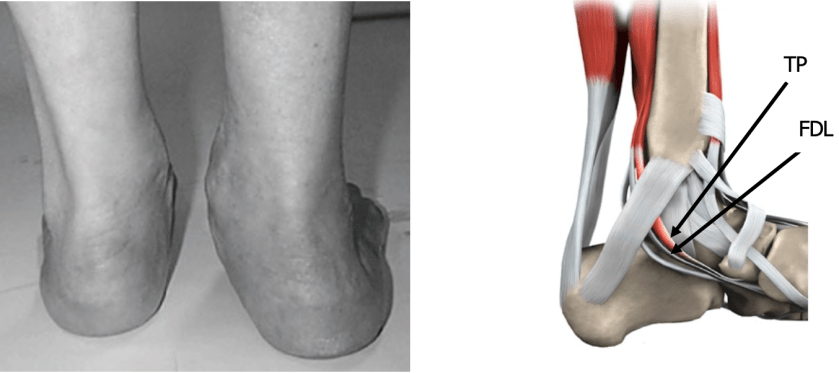
The tibialis posterior (TP) tendon is one of the major stabilising structures in the foot. It runs behind the bump on the inside of the ankle (the medial malleolus) and across the instep where it inserts. The main functions of the tendon are to support the arch and keep the foot turned inwards when walking. The TP can become damaged by wear and tear or acute trauma.
Initially, pain is felt along the length of the tendon (behind the medial malleolus), but as the problem worsens deformity becomes apparent and the foot flattens and turns outwards. Pain may develop on the outside of the ankle and if the deformity continues to worsen over time the joints in the hind foot become affected and can become arthritic. The surgical treatment is complex and depends on the location and severity of damage.
Non-Operative Management
In the early or mild stages of TP tendon dysfunction, simple painkillers, orthotics, and physiotherapy are used. Sometimes this is not sufficient and the problem progresses or the foot becomes arthritic. In this case surgery can help.
Operative Management
In most cases the tendon itself is repaired and needs to be strengthened by using another tendon, flexor digitorum longus (FDL). This tendon lies alongside tibialis posterior at the ankle and bends the small joints of the toes. Other tendons help to carry out this function and so the tendon is not really missed when it is used.
To improve the biomechanics of the tendon transfer the heel bone is moved towards the inside of the foot (calcaneal osteotomy), held with one screw and a plug is inserted into the subtalar joint to support the arch. The plug and screw are generally removed in a second operation when the tendon is strong enough, about 6 months after the first operation. This is a small day case operation and recovery is swift.
Triple Fusion
In more advanced cases, up to three of the joints in the foot can become arthritic. These joints (subtalar, talo-navicular, and calcaneo-cuboid) are fused using bone graft taken from either the heel or the hip bone. This is known as a triple fusion.
Risks & Complications
No surgery is risk free. The risks and complications will be assessed and discussed with you. There is always a small risk of infection, blood clots and anaesthetic problems and measures are taken to reduce these.
Specific risks include tendon re-rupture or progressive arthritis requiring further surgery, nerve damage resulting in numbness of the foot, wound or bone healing issues, and failure to relieve pain. Despite these risks, a satisfactory outcome is expected in 90% of cases.
Recovery Times :
The recovery from tendon reconstruction or fusion surgery is lengthy. You will spend 6 weeks in a cast and then undergo an intensive rehabilitation program as directed by your physiotherapist.
Hospital stay 2 nights
Rest & elevation 7-10 days
Crutches/frame 6 weeks
Plaster 6 weeks
Foot swelling 3 months
Implant removal 6 months
Time off work
– Seated 4-6 weeks
– Standing 3 months
Result times (pain relief & function)
– Good 3 months
– Better 6 months
– Best 12 months